Mostly because brains freak me out, and I've never been that comfortable with what to do with tubes and bolts sticking out the top of people's heads....
Here is a picture to tell you where the drain sits inside the brain:
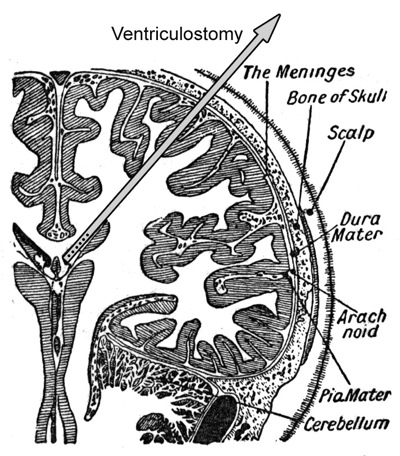 |
| source |
The external collections system of the brain is set to only drain if the pressure within the brain gets above a certain point. The drainage system has to stay level with the ear canal to monitor this pressure accurately. Our doctors have to move the procedure table up and down and back and forth all through the case. This means that not only are we giving medications, monitoring heart rate, blood pressure, oxygen, etc. Now we are freaking out on a drain that is vital to helping decrease injury to the brain. My shoulders are turning to earrings just thinking about this...
However, regardless of my wants and fears, my hospital has hired two new neuro surgeons, and signed a contract for two neuro interventional radiologists to work in our department...A neuro interventionalist puts a catheter in the femoral artery and threads it up to the brain to do interventions...Mostly put coils into vessels that are bleeding. Do you know the sort of confidence they must have to carry to put coils in a brain through a catheter that originates at the groin?
Ack.
The other thing that is stressing my fellow coworkers and me out is that while we have all been reading up on and taking skills tests on these neuro patients, we haven't had much real life experience. It's kind of like when you graduate nursing school and you have lots of head knowledge but can't put it all together easily. Only instead of working with a preceptor, we are wading through the trenches on call cases at night. Thus far we've learned that most patients don't tend to have crises in normal business hours. If the patient is in the ICU we can drag that nurse along with us, but if the patient is still in the ER, we are on our own. We've actually started adding a second call nurse to come in as a back up if the case is really hairy. We are all super excited about more call.
Not.
Anyway, Monday night as my shift was ending I found out we had an intracranial hemorrhage in the ER. "Don't panic, Dr. G is going to do it, and it's just diagnostic." That was good news for me as Dr. G is "my" doctor and he works much faster than the neuro interventionalists. Plus, I know him better (and he knows me) so we work better together. For instance, he understands that I'm going to get snappy and possibly tell him to "be quiet and let me catch up" with these urgent cases where everyone is rush rush rushing and I haven't even had time to give the patient medications, or if I have I haven't charted a single thing I've done, or "you are making me nervous positioning that table. I don't have my lead on yet." And he knows I don't want to get fried, so he would never xray while I am "naked." But again, these are all things I tend to get snippy about in these late cases. Especially considering I was hungry...
You have to understand that when an emergent case occurs during the day, even though I may be the only nurse in the room, there are at least three other nurses just outside my door. At night, I'm the only nurse unless the patient is from the ICU, and then I can drag that nurse along with me to the procedure. When things are going down, it's always best to have a pack mentality. You know, safety in numbers. The more people that I have in the room with me that meet my skill set, the better I feel...
I was surprised when I went to get the patient from the ER to see that she is only one month older than me. She has six children, the youngest of which is just a baby. She was actually alert and oriented, but she had "the worst headache of her life." She was walking into the grocery store that morning and her headache, which she'd had for three days, became so bad that she felt as if something exploded in her head. She called 911 and ended up with me that night. After chatting with her I learned that she had went to her doctor after she had her baby, and the doctor said her blood pressure was normal so she quit taking her medicine. She didn't understand that the blood pressure was normal BECAUSE she was on medicine.
Sometimes I get so frustrated with the ignorance of people. It all seems so pointless and at times just plain stupid. However, I also realize that a big piece of it is lack of proper education.
And the jaded nurse in me also realizes that another big piece is noncompliance. Unfortunately I see a lot more noncompliance than lack of education. Truthfully I think this was really a lack of understanding.
She was a never smoker, denied any drug use, occasional drinker with the brain of a 70 year old.
High blood pressure: The silent killer.
After the procedure was over her daughter had arrived. She looked about the age of my girls.
And she was scared to death. I pulled her mom's oxygen tubing off of her face and took her surgical hat that I had covering her hair off and encouraged the girl to chat with her mom to see that she was okay...She was being so good and so strong and trying so hard to hold the big pools of tears in her eyes back. Her voice was wobbly and her breath was shuddering.
For some dumb reason, I said "Baby it's okay. Your mommy is going to be okay. I promise."
No sooner did those words leave my mouth than I wanted to take them back. I can't make that promise! I've never made such a dumb promise in my life! I let my emotions get the best of me, and I made a rash statement.
Those words haunted me off and on throughout Monday night.
The next day we had to repeat part of the study to get a little clearer picture of one portion of her brain. Her daughter was not with her, but I learned that the little girl had spent the night at the hospital and was home resting. By the time we were complete with the follow up study, her daughter was back at the hospital. She rushed up and gave her mommy a kiss on the cheek after I quickly whipped as many tubes off of her mommy that I safely could.
I am not sure what the decision was based on our follow up films. I had read in the neuro surgeon's note that was written before our study that he was "asking for a repeat, with probable surgery in the morning." I didn't get to learn what the findings were because as soon as I returned to our department I had to tend to another patient who was having irregular heart beats. Then I had another patient in the ER that we had to go get and do a procedure on...
And then it was 7pm, and I had never even eaten lunch, so I simply clocked out and came home.
But my little momma has been on my mind. I pray that she's okay so that she can be a mommy to her six children.
P.S. I originally typed this post on Wednesday. On Thursday I went to check on her. She had gone through surgery to clip the aneurysm in her brain on Wednesday well. On Thursday she was alert and oriented and doing great. Hopefully she will have a full recovery.
4 comments:
Oh. My. Sad. Love the "shoulders are earrings' line. That's so me! and Teacups? we have not about 286 ish. Give or take a crack or chip...
I liked the shoulders as earrings line, too. I've never heard it put like that. Humorously accurate. And Dawn, I had to go back to your entry's comments to figure out what the 286 meant.
Andi, I am not crazy. A littled skewed, but not crazy - yet.
You poor thing! Of course you wanted to say that to the little girl.
In my humble opinion, as the wife of a soldier and someone who is constantly promising the kids that daddy will be ok, the relief brought by that promising something you can't possibly know, is sometimes worth the possible sour ending. In other words, if something does happen to daddy, it will be so incredibly horrible that the years of being lied to by their mother will most likely pale into insignificance. I'm sure it will be the same for the little girl, too.
Post a Comment